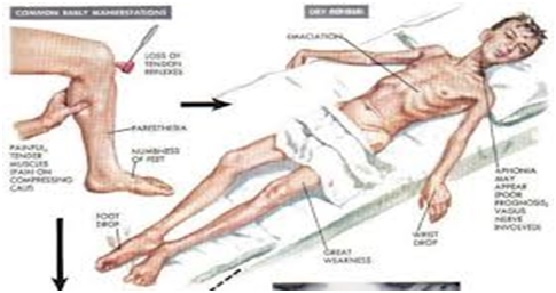
Thiamine Deficiency (Vitamin B 1)
Nutritional deficiencies are common after bariatric surgery, however, they are avoidable. There needs to be careful monitoring of nutrients. These include Iron, Vitamin B12, Vitamin B 1, Folic Acid and Vitamin D.
Thiamine is a water-soluble vitamin and is absorbed in the small intestine. Approximately 5 mg of thiamine is absorbed through the small intestines. The body cannot produce thiamine and can only store up to 30 mg. of it in the body’s tissues. Thiamine is concentrated in the skeletal muscles. Lesser amounts are found in the brain, heart, liver and kidneys. The half-life of thiamine is approximately 9-18 days and is excreted by the kidneys.
Morbidly obese patients may have poor dietary habits with increased calories and refined carbohydrates. Further, they often use diuretics (water pills) for the control of other medical conditions. This can contribute to thiamine deficiency. One study of over 300 morbidly obese patients scheduled for weight-reduction surgery, 15% were shown to have low pre-operative thiamine levels. Combined with higher bodily demands due to surgery, along with rapid weight loss postoperatively, and less absorptive area can lead to severe deficiency. In addition, deficiency can occur by not consuming enough Vitamin B1 through the diet or can result not only from bariatric surgery, but has been found to be associated those on dialysis, over-active thyroid, cancer, pregnancy, lactation, fever, vomiting and alcohol dependency. Thiamine deficiency can lead to serious complications involving the nervous system, brain, muscles, heart and intestines. This can be evidenced within 18 days. With adequate thiamine replacement, symptoms can disappear within 24 hours.
Thiamine deficiency has been associated with three disorders. They are:
- Beriberi
- Wernicke-Korsakoff syndrome
- Leigh’s syndrome
This is described as dry or wet. Dry Beriberi is the development of bilateral peripheral neuropathy with both sensory and motor impairments, mostly affecting distal extremities. Wet beriberi includes neuropathy as well with cardiac involvement with weakened heart muscle, congestive heart failure, lower extremity edema and tachycardia (fast heart rate). Symptoms include a burning sensation in the extremities, weakness, and balance problems. Further, some studies have suggested that patients with heart failure treated with loop diuretics (type of water pill), may become thiamine deficient.
Wernicke-Korsakoff syndrome
This is one of the most notable neurologic complications of thiamine deficiency. This refers to two different syndromes, each representing a different stage of the disease. Wernicke’s encephalopathy is an acute syndrome requiring emergent treatment to prevent death and neurologic deterioration. This is almost always a consequence of alcoholism. Korsakoff’s syndrome refers to a chronic neurologic condition that occurs as a consequence of Wernicke’s encephalopathy.
Patients who are diagnosed with low thiamine levels prior to surgery should be prescribed Thiamine 100 mg. 2x daily for one month or until thiamine levels are within normal limits. Further, those patients with prolonged vomiting and/or diarrhea should also receive thiamine. Thiamine levels pre and post-surgery should be monitored.
Normal daily thiamine requirements are 1.2 mg daily for adult men and 1.1 mg. daily for adult women. The kidneys can rapidly clear almost all excess thiamine therefore; there is no concern for toxicity.
Foods rich in thiamine include:
- Whole grain foods
- Meat/fish/poultry/eggs
- Milk and milk products
- Vegetables (particularly green, leafy vegetables, beets)
- Legumes (lentils, soybeans, nuts, seeds).
Bariatric patients should have routine follow up with their providers for assessment overall health, to assess for any evidence of nutritional deficiencies, assess co-morbidities, undergo physical examinations, as well as regular blood analysis. In addition, close followup with dietitians is recommended for nutritional guidance.
See image below: